Data-Driven Decisions: Using NHS Metrics to Improve Respiratory Outcomes
In respiratory care, the gap between what we know and what we do is often measured in data we're not quite using yet. The NHS collects extraordinary amounts of information on admissions, readmissions, wait times, prescribing patterns and clinical deterioration. What's harder is turning that data into decisions that change outcomes on the ground.
This isn't about dashboards for the sake of dashboards. It's about understanding where care is failing, why it's failing, and what levers exist to fix it. For clinicians stretched across multiple sites, for patients navigating fragmented pathways, and for Life Sciences teams trying to support improvement: the same datasets can answer very different questions.
What the Data Actually Shows
The numbers paint a clear picture of inequity. Hospital admission and death rates for respiratory disease vary significantly across Integrated Care Systems, with six of the 10 highest-burden ICSs located in the North East and North West. Nine of the 10 lowest-burden systems sit in London, the South East and South West.
Deprivation drives much of this. The three most deprived ICSs in England all fall within the top 10 for respiratory hospital admissions and deaths. What that means in practice is that postcode determines not just access to care, but likelihood of survival.

Wait times tell a similar story. The percentage of respiratory patients seen within the 18-week standard ranges from over 80% in the best-performing ICSs to under 50% in the worst. Workforce ratios: particularly consultants per population: correlate closely with performance. Where there are fewer specialists, patients wait longer. And while they wait, conditions worsen.
Early Warning Systems and Clinical Deterioration
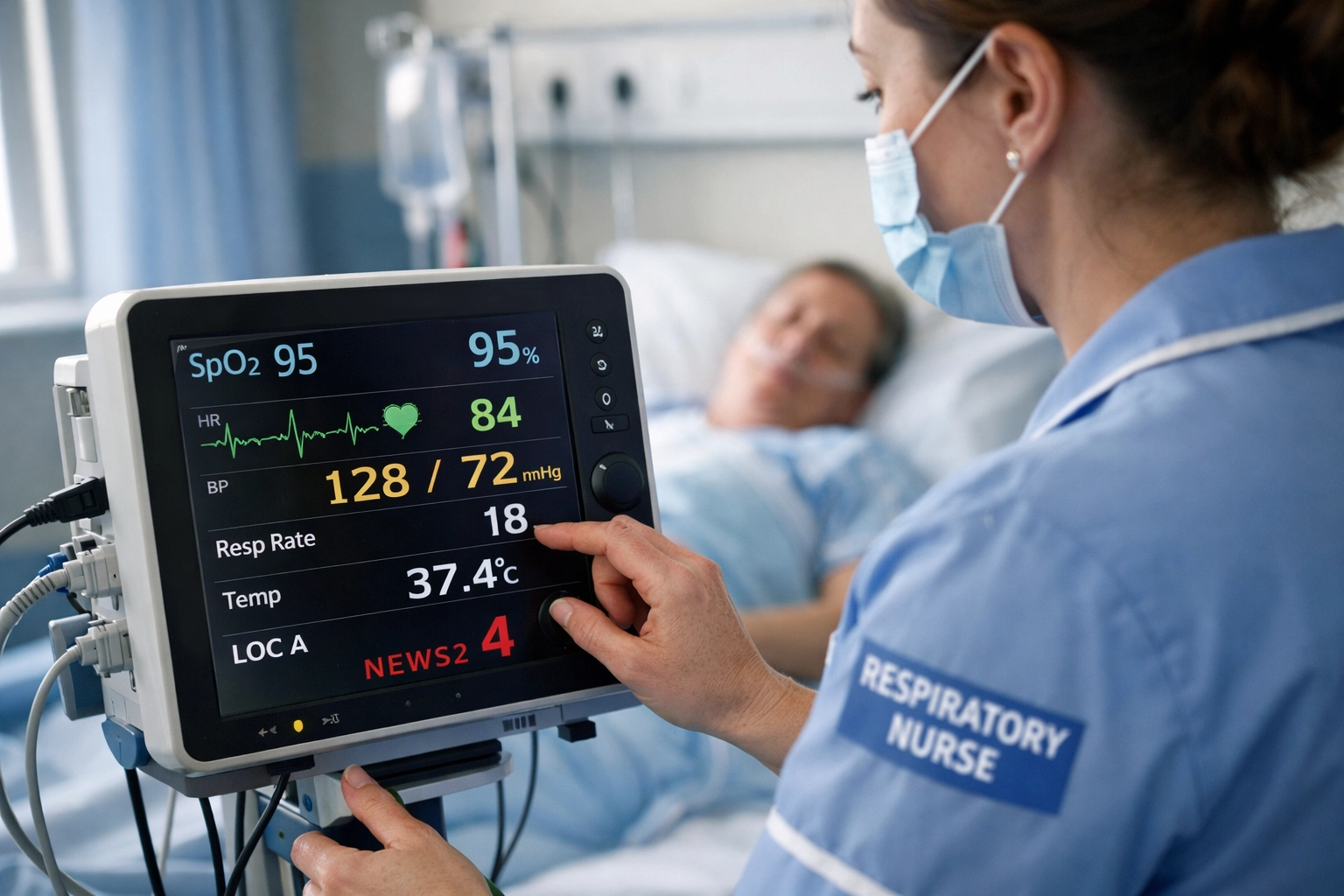
One of the more operationally useful datasets is the National Early Warning Score 2 (NEWS2), deployed in 76% of acute hospital trusts across England. NEWS2 uses six vital sign parameters: respiratory rate, oxygen saturation, heart rate, blood pressure, temperature and neurological status: to categorise patients at risk of deterioration.
A score of 5 or more triggers an urgent clinical response. A score of 7 or more requires emergency intervention and continuous monitoring. What this does, in effect, is standardise risk assessment across wards and trusts. It creates a shared language for escalation, which matters when respiratory patients can deteriorate quickly and unpredictably.
The limitation is that NEWS2 only works if it's acted on. Data collection without decision-making infrastructure just creates noise. The metric is most effective in trusts where there are clear escalation pathways, senior clinical oversight and adequate staffing to respond in real time.
Readmissions and the 30-Day Window
Readmission within 30 days of discharge is one of the most stubborn metrics in respiratory care. It reflects not just the severity of disease, but the quality of discharge planning, access to community support and continuity between secondary and primary care.
Respiratory conditions are the third biggest killer in the UK and consume the second-largest portion of NHS bed days. Much of that demand is preventable. Patients discharged without follow-up, without medication reconciliation, without clear escalation plans: they come back. Often sicker than when they left.
Large-scale outcome tracking reveals that post-discharge care is where systems fracture. GP capacity, access to respiratory nurses, pulmonary rehabilitation waiting times: all of these variables show up in the 30-day readmission data. Fixing them requires coordination that most ICSs are still building.
How Data Translates into Practice Change
Knowing where the problems are is useful. Knowing what to do about them is harder. But there are examples of metrics driving tangible shifts.
One is SABA overprescribing. Short-acting beta-agonist inhalers are frequently prescribed at volumes that indicate poor asthma control. Data on prescribing patterns has informed the rollout of new NICE, SIGN and BTS asthma guidelines, which emphasise MART (Maintenance and Reliever Therapy) and AIR regimes.
In practice, this means using prescribing data to identify patients at risk, then proactively reviewing and adjusting treatment. It's a simple intervention with significant impact: fewer exacerbations, fewer admissions, better long-term control.

Another example is resource reallocation based on deprivation and burden data. Asthma + Lung UK has called for respiratory conditions to be prioritised in the NHS 10-year plan, with targeted investment in the highest-need ICSs. This isn't about blanket funding. It's about using data to direct resources to the places where they will have the greatest effect.
Winter Pressures and Year-Round Care
Respiratory demand spikes every winter, but the data shows that much of the crisis is predictable. Metrics tracking seasonal admissions, readmissions and workforce strain have informed the case for year-round community respiratory programmes: annual reviews, vaccinations, early intervention for exacerbations.
What this looks like on the ground is embedding respiratory care into primary care networks, not just acute settings. It's pulmonary rehab that runs continuously, not just when bed pressures ease. It's proactive outreach to high-risk patients before flu season, not reactive admissions in January.
The shift is incremental, but the data makes the case clearly: prevention is cheaper and more effective than crisis management. The challenge is that prevention requires investment now for savings later: a harder sell in a system under immediate pressure.
The Economic Argument
Asthma costs the NHS £3 billion annually. COPD costs £1.9 billion. Both figures are dominated by emergency admissions and long-term complications that could, in many cases, have been avoided.
The economic data strengthens the clinical case. Reducing admissions through better primary care, better discharge planning and better use of data doesn't just improve outcomes: it frees up capacity. It allows trusts to manage elective workloads, reduces winter bed shortages and improves staff morale by reducing crisis-driven work.
For Life Sciences, this data also clarifies where support is most needed. Diagnostic tools, remote monitoring technologies, adherence platforms: all of these have value, but only if they're deployed in the right places, to the right populations, with the right clinical infrastructure around them.
What Data Can't Do
Metrics are tools, not solutions. They identify problems but don't fix them. And there's a risk, particularly in stretched systems, that data becomes performative: collected because it's required, reported because it's measured, but not actually used to change practice.
What patients and clinicians often describe is data fatigue. More dashboards, more audits, more reporting requirements: without corresponding improvements in care. The value of metrics lies in their translation into action. Without that, they're just documentation.
There's also the question of what gets measured. Readmission rates, wait times, mortality: all important. But harder-to-quantify outcomes like quality of life, symptom control between exacerbations, patient confidence in self-management: these matter just as much, and they're harder to track at scale.
Using Data Well
The ICSs and trusts that use respiratory data most effectively tend to share a few characteristics. They have clinical leadership that understands both the data and the operational context. They have MDT structures that allow metrics to inform frontline decision-making. And they have a culture that treats data as insight, not compliance.
In practice, that means respiratory leads who can interpret prescribing data and translate it into changes in formulary or pathways. It means using readmission metrics to redesign discharge processes, not just report them upward. It means linking workforce data to service planning, so that capacity follows demand.
It also means being realistic about what's achievable. Not every intervention will work. Not every data point will lead to immediate improvement. But the systems that get better are the ones that learn from their own metrics and adapt accordingly.

Moving Forward
The datasets exist. The analytical capacity exists. What's often missing is the space to think, the time to reflect and the infrastructure to act. Data-driven decisions require clinical time, MDT coordination and system-level buy-in: all of which are in short supply.
But the direction is clear. Respiratory care improves when data informs practice, when metrics drive resource allocation and when insights translate into clinical change. The challenge is building the conditions that make that possible: not just in high-performing ICSs, but everywhere.
We bring together NHS respiratory leads, patient advocates and Life Sciences teams to share insight and improve practice. If this resonates with the challenges you're facing, join our community or come to our next Round Table event to continue the conversation.







Responses