The Community Shift: How the 10-Year Health Plan Redefines Respiratory Care

The landscape of respiratory care in the UK is currently undergoing its most significant structural shift in a generation. With the unveiling of the 10-Year Health Plan, the focus has moved decisively away from the traditional hospital-centric model toward a system grounded in local communities. This is not merely a change in geography; it is a fundamental redesign of how the NHS intends to manage a disease area that affects one in five people and remains the third leading cause of death in England.
For those working within Integrated Care Systems (ICSs) and Primary Care Networks (PCNs), the plan represents a formal acknowledgment of a reality they have navigated for years: respiratory conditions are often managed most effectively when interventions happen early, locally, and consistently.
A System Under Pressure
The necessity for this shift is evidenced by the data. While general hospital admissions have grown at a steady rate, admissions specifically for lung disease have risen at three times that pace. This trajectory is unsustainable for secondary care and, more importantly, often represents a failure in the earlier stages of the patient pathway. When a person with a chronic respiratory condition reaches the point of emergency admission, it frequently suggests that opportunities for intervention in the community were either missed or unavailable.
The 10-Year Health Plan aims to address this by reallocating resources and clinical focus. The objective is to move care out of the acute setting and into the neighborhood. In practice, this means transitioning from a model of "crisis management" to one of "chronic stability."

Neighborhood Teams: The New Front Line
The cornerstone of the community shift is the empowerment of neighborhood teams. These multidisciplinary groups: comprising GPs, community nurses, pharmacists, and allied health professionals: are being positioned as the primary coordinators of respiratory care.
What this looks like on the ground is a move toward more proactive, data-driven management. Rather than waiting for a patient to present with worsening symptoms, neighborhood teams are being encouraged to use integrated patient data to identify those at high risk. This allows for scheduled reviews and adjustments to care plans before a respiratory event occurs.
For the clinician, this requires a higher degree of connectivity between primary and secondary care. The plan emphasizes that neighborhood teams must have seamless access to specialist advice without necessarily referring the patient back into a hospital waiting list. This "specialist-to-primary" knowledge transfer is essential for managing complex cases within a community setting.
The Diagnostics Gap and Early Intervention
One of the most significant barriers to effective community-based respiratory care has historically been the "diagnostics gap." Many respiratory conditions are diagnosed late, often after significant lung function has already been lost. The 10-Year Health Plan prioritizes closing this gap through increased access to testing within the community.
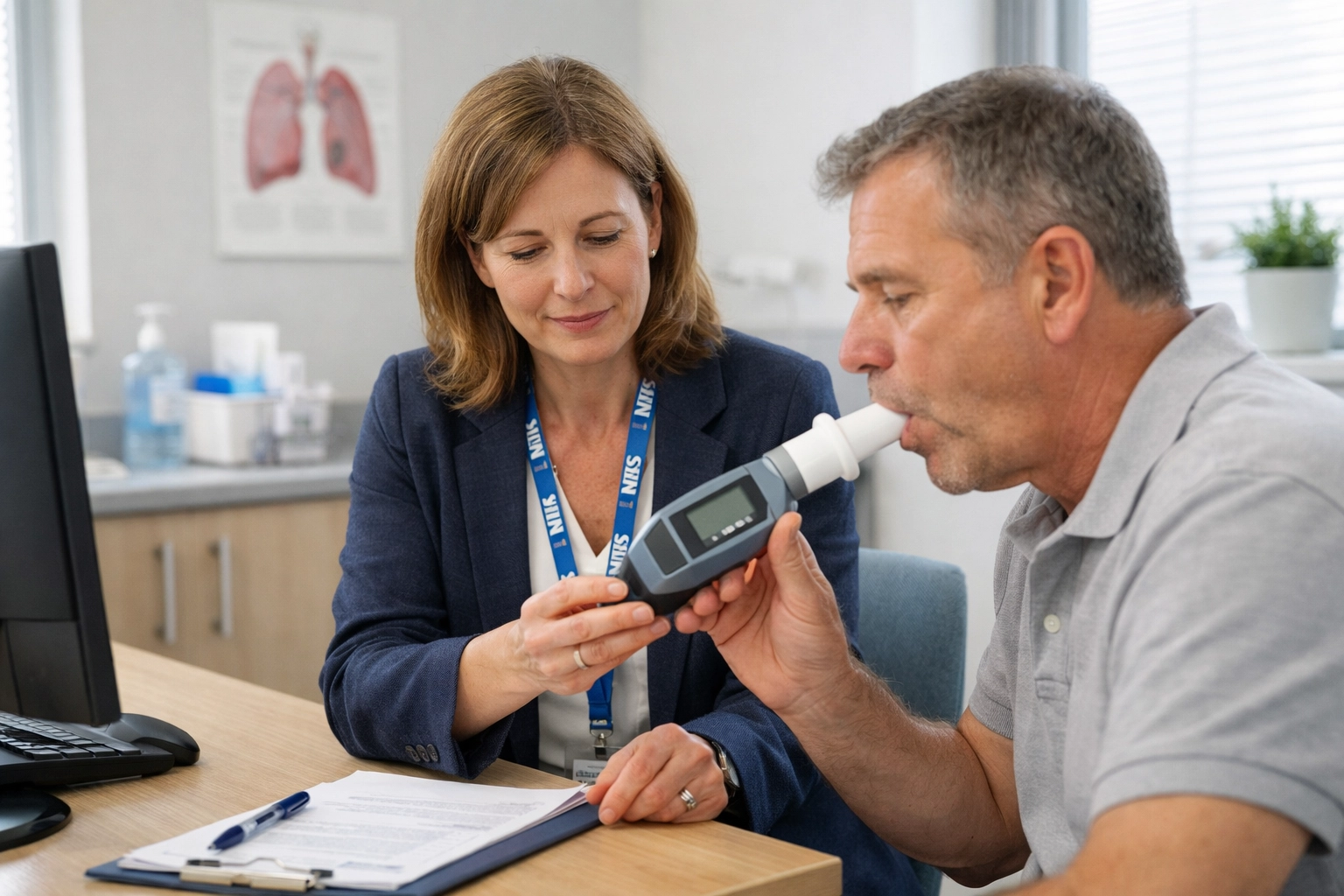
In practice, this means a renewed focus on spirometry. For several years, access to high-quality, diagnostic-standard spirometry has been inconsistent across different regions. The plan envisions a system where these diagnostic tools are standard features of local health hubs, allowing for earlier identification of conditions.
What this looks like on the ground is a shift in the patient's journey. Instead of a patient traveling to a distant hospital for a diagnostic appointment, these assessments take place in local clinics or diagnostic centers. Earlier diagnosis allows for earlier intervention, which is the most effective way to slow disease progression and maintain a person's quality of life.
Addressing the Environmental Drivers of Health
A notable aspect of the 10-Year Health Plan is its recognition that respiratory health is not determined solely within the walls of a clinic. The plan looks outward at the social and environmental factors that drive respiratory illness.
There is a direct correlation between housing quality and lung health. The plan explicitly links respiratory outcomes to the living environment, requiring social landlords to act promptly on issues such as damp and mould. From a strategy perspective, this represents an integration of health policy with housing and environmental standards.
In practice, healthcare professionals are increasingly seeing the impact of "fuel poverty" and poor housing on their patient populations. By addressing these root causes, the NHS aims to reduce the underlying triggers of respiratory flare-ups. This holistic approach recognizes that a clinical pathway is only one part of the solution; the environment in which the person lives and breathes is equally critical.
Digital Transformation and the 2035 Vision
Technology is the thread intended to pull these community-based services together. The 10-Year Health Plan sets an ambitious target: by 2035, wearables and remote monitoring are expected to be standard in preventative and chronic care.
For respiratory care, this digital shift is particularly relevant. Remote monitoring allows for the tracking of lung function and symptom patterns in real-time. What this looks like on the ground is a patient using a connected device at home, with the data being monitored by a community respiratory team. If the data shows a decline in stability, the team can intervene immediately.
This move toward self-management is supported by the expansion of digital tools for pulmonary rehabilitation. By making these services available online or via mobile platforms, the plan seeks to improve uptake and completion rates for rehabilitation: a service that is evidence-based but historically underutilized due to travel and access barriers.

Tackling Health Inequalities
Perhaps the most urgent driver of the community shift is the need to address health inequalities. Respiratory disease is a primary contributor to the gap in life expectancy between the wealthiest and most deprived communities in the UK. Lung conditions are strongly linked to deprivation, and those in poorer areas are more likely to be diagnosed late and experience worse outcomes.
The 10-Year Health Plan places a heavy emphasis on reducing premature deaths in these communities. By moving care into the heart of these neighborhoods, the NHS aims to reach populations that have traditionally been underserved by hospital-based models.
What patients and clinicians often describe in these areas is a sense of being "lost in the system." A localized, community-led approach aims to provide a more visible and accessible point of contact, ensuring that those at the highest risk receive the most intensive support.
The Role of the Wider Network
As these strategic changes take hold, the role of collaboration becomes even more vital. The transition from hospital to community requires a shared understanding between NHS leadership, frontline clinicians, and the Life Sciences sector. No single part of the system can deliver this shift in isolation.
The Respiratory Network exists to facilitate these conversations, ensuring that as pathways change, the insights of those with lived experience and those delivering care are heard. We are moving toward a future where "respiratory care" is synonymous with "community care," and success will be measured by our ability to keep people breathing well in their own homes, rather than treating them in a hospital ward.

Conclusion: A Measured Transition
The 10-Year Health Plan is an ambitious roadmap, but its success depends on practical, grounded implementation. Moving care closer to home is a logical step, yet it requires significant investment in workforce, diagnostics, and digital infrastructure. It also requires a shift in mindset: from seeing the hospital as the center of the healthcare universe to seeing it as a specialized resource for those who truly need it.
As we look toward the next decade, the goal is a respiratory pathway that is proactive, equitable, and firmly rooted in the local community.
Join the Conversation
Are you involved in redesigning respiratory pathways within your ICS or PCN? We invite you to join our community of professionals dedicated to improving respiratory outcomes across the UK.
- Become a Member: Join The Respiratory Network to access exclusive insights and connect with peers. Join here
- Follow Us: Stay updated on the latest strategy and leadership insights by following us on our social media channels.
- Attend Our Next Event: Join us for our upcoming Round Table to discuss the practicalities of the 10-Year Health Plan. View events
Medical Disclaimer: The information provided in this blog is for informational purposes only and does not constitute medical advice. Always seek professional clinical guidance for medical conditions.







Responses