Bridging the Diagnostic Gap: Why Spirometry and FeNO Are Non-Negotiable in 2026

The landscape of respiratory care in 2026 is defined by a paradox. On one hand, we are witnessing an era of unprecedented therapeutic potential, with new treatments reaching the frontline of the NHS. On the other, the foundational step of the patient journey: accurate, timely diagnosis: remains a significant hurdle. For clinicians, commissioners, and patients alike, the "diagnostic gap" is not merely a statistical backlog; it is a clinical risk that dictates the quality of life for millions.
In practice, we are seeing a shift in how the system views objective testing. The reliance on symptomatic diagnosis, once a necessity during periods of high system pressure, is increasingly recognised as insufficient. To truly transform respiratory outcomes, the integration of Spirometry and Fractional Exhaled Nitric Oxide (FeNO) testing must be treated as a non-negotiable standard of care rather than an optional luxury.
The Reality of the Diagnostic Backlog
What we see on the ground is a system still working to find its equilibrium. Recent reports have highlighted the urgent need for dedicated funding to clear the diagnostic backlog that has persisted for several years. In certain regions, the call for emergency investment: such as the recent £3m appeal in Scotland: underscores the depth of the challenge. These are not just figures on a spreadsheet; they represent thousands of individuals living with breathlessness without a confirmed cause.
When diagnosis is delayed, the system defaults to "best guess" prescribing. While this may offer temporary relief, it often leads to a cycle of repeat consultations and ineffective treatment plans. What patients and clinicians often describe is a sense of frustration when symptoms persist despite multiple rounds of medication. Bridging this gap requires more than just equipment; it requires a focused strategy on pathway innovation and workforce support.

Why Objective Testing Matters: The Complementary Duo
It is often asked why both Spirometry and FeNO are necessary. To understand this, we must look at what these tests tell us about the biological reality of the lungs. They are complementary, not interchangeable.
Spirometry remains the gold standard for assessing mechanical lung function. It measures the "plumbing": how much air a person can breathe out and how quickly they can do it. It identifies airflow obstruction, which is critical for diagnosing conditions like COPD and monitoring the progression of chronic disease. However, as many clinicians are aware, a patient with asthma can often produce a normal spirometry result between episodes, even while inflammation is present.
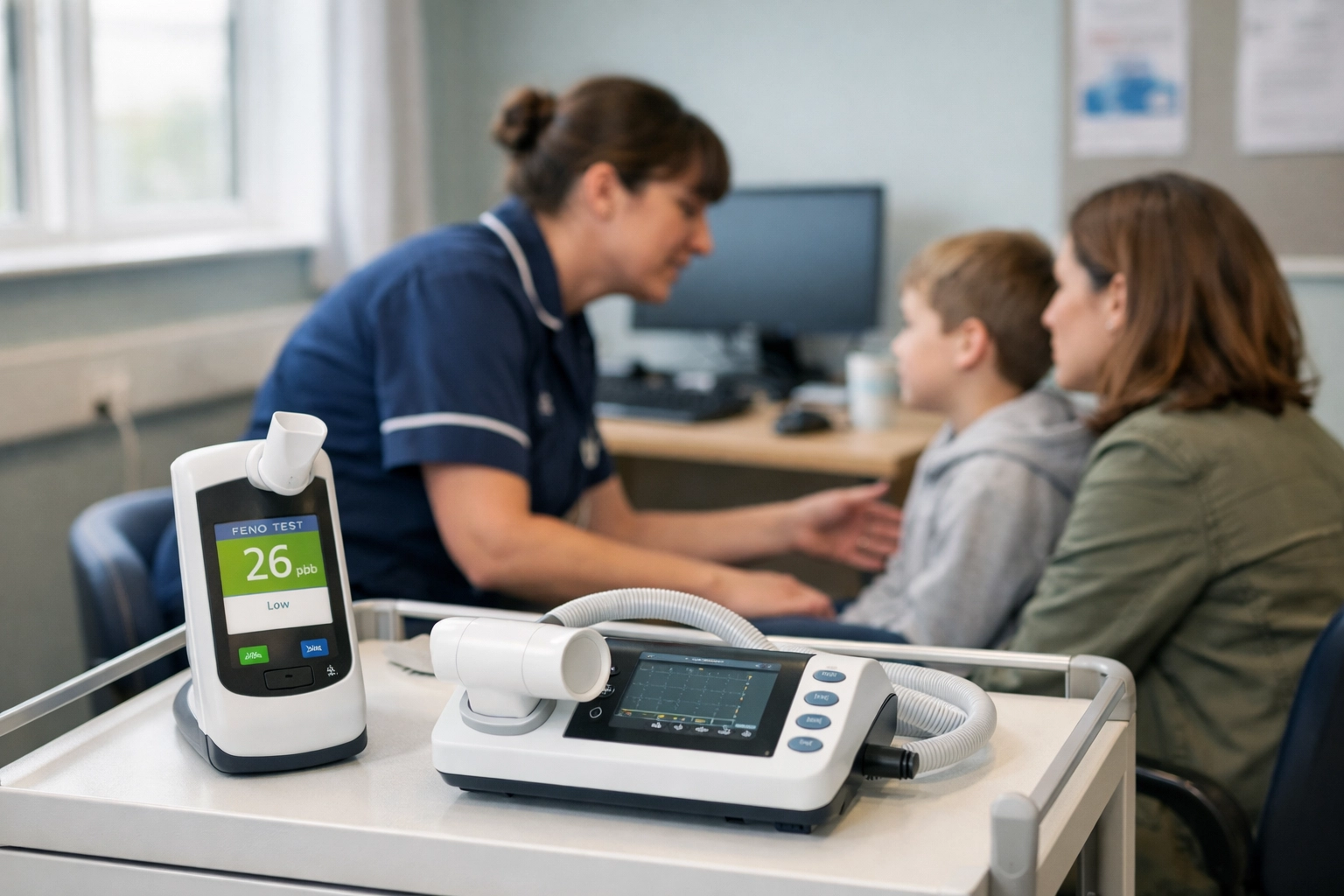
This is where FeNO testing becomes essential. FeNO measures the "fire": the level of eosinophilic inflammation within the airways. By measuring the concentration of nitric oxide in exhaled breath, clinicians can detect active inflammation that spirometry might miss. Together, these tests provide a 360-degree view of the patient’s respiratory health.
The Pediatric Imperative: Moving Beyond the Reliever
Perhaps the most urgent area for diagnostic reform is in pediatric care. Recent clinical observations have highlighted a concerning trend: the over-reliance on reliever inhalers in children. Without objective testing, it is incredibly difficult to distinguish between different types of childhood wheeze or to confirm an asthma diagnosis with certainty.
In practice, this often leads to children being prescribed "blue" inhalers as a primary response to breathlessness. While these provide immediate relief, they do not treat the underlying inflammation. Over-reliance on these medications is a known risk factor for severe exacerbations. By implementing FeNO and spirometry earlier in the pediatric pathway, we can ensure that children are started on the correct preventative treatments from day one, potentially altering their long-term health trajectory.
Pathway Innovation and the Workforce Challenge
Integrating these tests into every Primary Care Network (PCN) or Integrated Care System (ICS) is not without its hurdles. The primary barrier is often not the cost of the devices themselves, but the capacity of the workforce to deliver them.
Performing high-quality spirometry is a skilled task that requires specific training and certification. Similarly, interpreting FeNO results within the context of a patient's clinical history requires time and expertise. What we see in the most successful pathways is a commitment to "diagnostic hubs": centralised locations where patients can access all necessary tests in a single visit, supported by a workforce that has protected time for testing and review.
This model of pathway innovation reduces the burden on GP surgeries and ensures that the data being collected is accurate and actionable. It also allows for better "medication stewardship," ensuring that the right people get the right treatment, thereby reducing waste and improving the sustainability of care.
The Role of Life Sciences and Collaboration
The shift toward objective testing is also a priority for the Life Sciences sector. For innovation in therapeutics to be effective, patients must be correctly stratified. A treatment designed to target specific inflammatory pathways is only as good as the diagnostic framework that identifies the patients who will benefit from it.
Collaboration between the NHS and industry partners is vital in this regard. Whether it is through supporting workforce training or developing more portable, user-friendly diagnostic tools, the goal is the same: a respiratory service where "knowing" replaces "guessing."
Looking Ahead: A Purposeful Approach
As we move through 2026, the goal for the respiratory community is clear. We must move toward a future where a diagnosis of asthma or COPD is always backed by objective data. This is not about adding complexity to the system; it is about providing the clarity that clinicians need to make confident decisions and that patients need to feel secure in their care.
What patients often tell us is that receiving a definitive diagnosis is the point at which they finally feel in control of their condition. By prioritising Spirometry and FeNO, we are not just measuring lung function; we are providing the foundation for better lives.
Medical Disclaimer: The information provided in this blog is for informational purposes only and does not constitute medical advice. Always seek professional clinical guidance for medical conditions.
Join the Conversation
The Respiratory Network is dedicated to fostering collaboration across the UK respiratory community. We invite you to join our growing network of clinicians, patient advocates, and life sciences professionals to stay informed on the latest diagnostic standards and pathway innovations.
- Follow us on social media for more updates on respiratory diagnostic standards and upcoming events.
- Explore our Post Sitemap to read more insights into the future of respiratory care.
- Connect with colleagues in our Community Forum.







Responses