Beyond the Pilot: Scaling Digital Tools into Standard NHS Respiratory Services
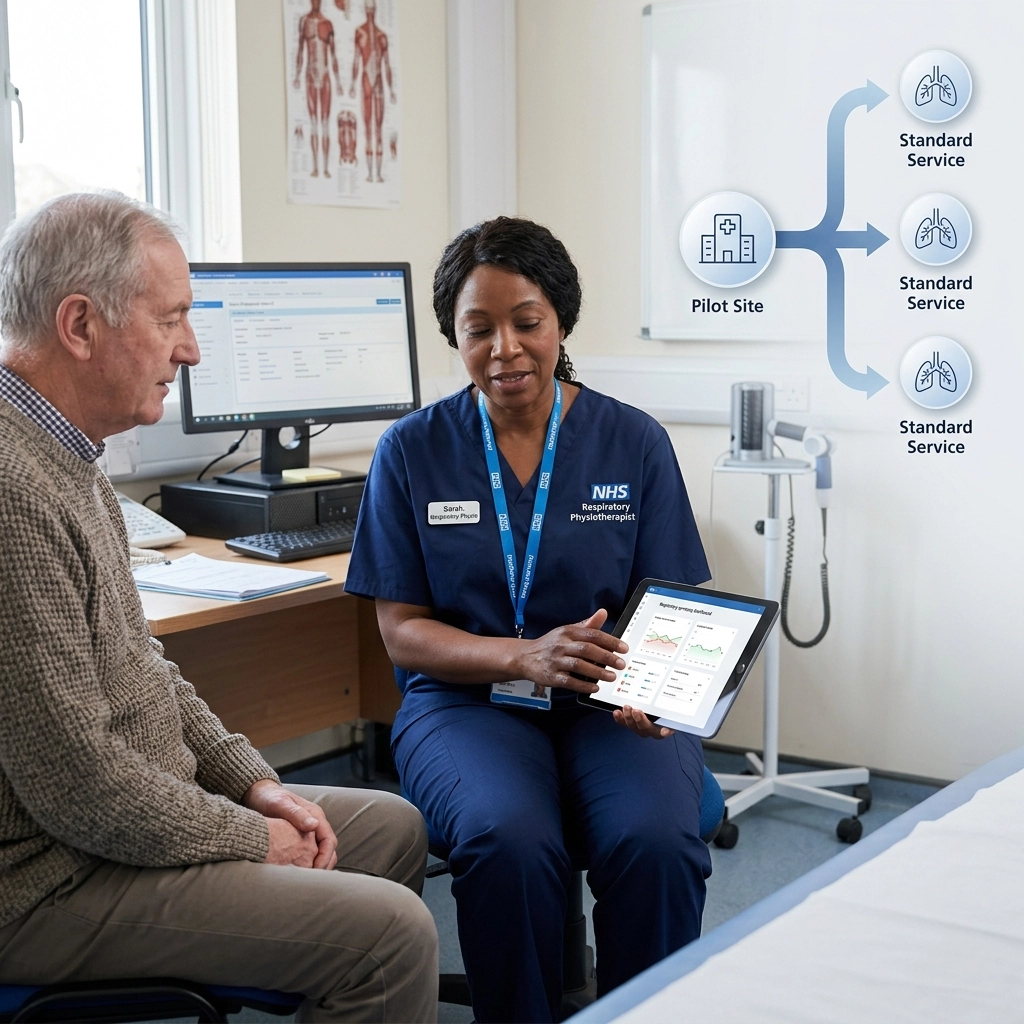
In the world of NHS respiratory services, we often talk about "pilot-itis." It is that familiar cycle where a new digital tool, a smart inhaler, a remote monitoring app, or an AI-supported triage system, is launched in a small corner of a Trust or a single PCN. The initial data is often encouraging: patients feel more supported, clinicians may see fewer emergency admissions, and the tech appears to do what it was designed to do.
Then, the pilot funding ends. The project enters a "review phase," and more often than not, it quietly disappears.
If we are going to make progress in respiratory care UK, we need to move beyond the excitement of something "new" and look at the practical work of making these tools part of standard, everyday practice. Digital respiratory monitoring should not be something only available to patients in certain postcodes; it needs to sit properly within the pathway, alongside the tools and processes teams already use.
The Evidence is Already Here
We aren't starting from scratch. Across the UK, there are already models of what happens when digital tools are integrated at scale rather than kept in the pilot lane.
Take the example of NHS Wales. They did not just test a digital therapeutics toolkit; they achieved 100% adoption across every GP practice and hospital in the country. This was not only an IT success. Patients reported a 41% improvement in wellness scores within four months. There was also a 36% reduction in GP visits and a 19% drop in A&E admissions.
Similarly, in Hull and East Yorkshire, an AI-enabled support system for COPD has been linked with a 40% reduction in hospital readmissions since early 2023. These are not just interesting results; they give a useful sense of what scale can look like in practice.

Moving from "Gadget" to "Clinical Intervention"
One of the biggest hurdles in scaling digital health is the way we perceive the technology. Too often, smart inhalers or remote monitoring apps are viewed as "patient education" or a "nice-to-have" add-on.
In practice, it may be more helpful to think about digital monitoring as part of service delivery rather than a bolt-on extra. If a smart inhaler can track technique, in a context where many patients use their devices incorrectly, that tool can support the kind of review that would otherwise rely on face-to-face time. When digital tools flag a change in symptoms or use patterns before a patient feels unwell, that can help teams respond earlier.
When we shift the perspective from "tracking a patient" to "supporting a pathway," the case for scaling becomes easier to understand. It moves away from being seen as an innovation project and closer to core service delivery.
The Integration Challenge: Beyond the App
Scaling technology is rarely about the software itself; it is about the "plumbing" of the NHS. For a digital tool to become standard care, it must be embedded into the local clinical protocols. This means having robust Standard Operating Procedures (SOPs) that dictate exactly what happens when a digital alert is triggered.
Questions we often hear from clinicians on the ground include:
- Who monitors the dashboard?
- Does this alert go to the GP, the respiratory nurse, or the integrated care board (ICB) hub?
- How does the data flow back into the primary care record without manual entry?
Without clear answers to these questions, even the best technology becomes a burden rather than a benefit. Integrated care systems (ICSs) have a unique opportunity here to standardise these pathways. Instead of five different PCNs using five different monitoring tools, the ICS can provide a unified framework that ensures data is actionable.
Workforce and the "Human" Element
We cannot discuss digital transformation without acknowledging the respiratory workforce. There is a valid fear that more data equals more work. If we give 1,000 patients smart inhalers, does that mean a specialist nurse now has 1,000 more data points to check every morning?
Actually, the goal of scaling digital tools should be the opposite: workforce sustainability.
By using remote monitoring to identify who is stable and who is deteriorating, we can move away from the "every six months" review model. Instead, we can focus our highly skilled clinicians on the patients who actually need them today. It allows for a move toward "proactive" rather than "reactive" care. Digital tools don't replace the respiratory nurse; they ensure the nurse's time isn't wasted on patients who are managing perfectly well.

Addressing Health Inequalities
As we scale, we have to be incredibly careful not to bake in further inequalities. There is a risk that digital tools only reach the "digitally literate" or those with the latest smartphones.
Pathway excellence means ensuring that digital transformation includes everyone. This might look like providing devices to those in lower socioeconomic groups or ensuring that remote monitoring platforms are accessible to people for whom English is a second language. If we only scale digital tools in affluent areas, we are failing the very populations that suffer the most from respiratory disease and air pollution.
Practical Steps for Scaling
If you are a clinical lead or a commissioner looking to move from a pilot to a standard service, here is what we’re observing works:
- Define the Goal Early: Are you trying to reduce A&E admissions, improve inhaler technique, or free up specialist nurse time? Your aim determines what you measure.
- Co-production matters: Involve patients and frontline staff from day one. If the app is too clunky for an 80-year-old with COPD, or the dashboard is too complex for a busy GP, it is unlikely to work at scale.
- Think About the Long-term: Plan for the "post-pilot" funding before the pilot even starts. Work with Life Sciences partners to understand how the service can be sustained through standard NHS procurement or value-based healthcare models.
- Integration with Existing Systems: Ensure that the tool talks to EMIS, SystmOne, or whatever EPR your Trust uses. Interoperability is a big part of scaling.
A Note on Clinical Safety
Please note that the information provided in this blog is for educational and networking purposes and does not constitute medical advice. Any decisions about care should be made by qualified healthcare professionals based on individual circumstances. The Respiratory Network does not endorse specific products, and any pathway design should align with relevant guidance and local governance processes.
What Does the Future Look Like?
We are moving toward a "One Airway" approach where digital tools do not just monitor a single condition, but look at the patient more holistically by connecting asthma, allergies, and even cardiac health. The technology exists and the evidence base is growing. The real question is how services make the shift from repeated trials to something more consistent and sustainable.
At The Respiratory Network, we think these conversations work best when different parts of the system are in the room together. Whether you are in Life Sciences, a clinical lead, or a patient advocate, there is value in working through these questions together.
Join the Conversation
Are you working on a digital project that is difficult to scale? Or have you seen what helps a pilot become part of standard care? We would be interested to hear your perspective.
- Become a Member: Join our community to connect with others working across respiratory care. Register here.
- Join our Forums: Continue the conversation in our Forums.
- Attend the Round Table: We will be exploring pathway innovation at our upcoming event on June 24th. Find details here: The Respiratory Network Round Table 2026.
Scaling digital tools isn't just about the technology: it's about the people, the pathways, and the commitment to making NHS respiratory services fit for the 21st century. Let's move beyond the pilot, together.







Responses