Lung Training: Can Microbes Actually ‘Teach’ Our Lungs to Resist Allergies?
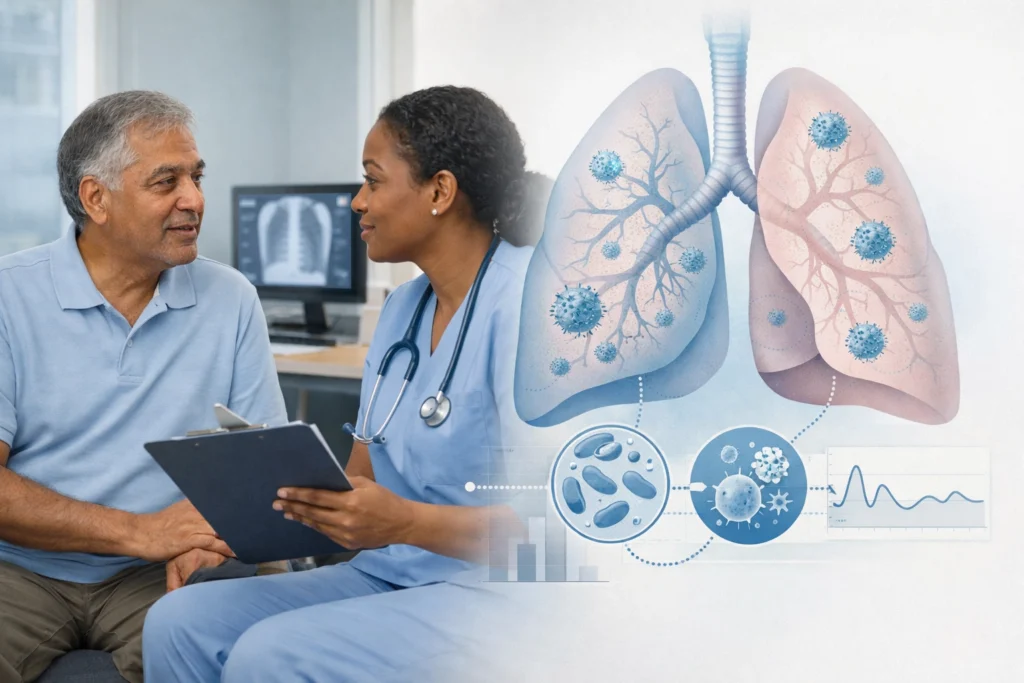
The rise in respiratory allergies and asthma across the UK presents a persistent challenge for the NHS. For decades, the prevailing understanding of allergic responses focused almost exclusively on the immune system: the white blood cells that identify and attack perceived threats. However, recent breakthroughs are shifting this perspective toward the "structural" environment of the lung itself.
New research, most notably from the Pasteur Institute, suggests that our lungs may undergo a form of "training." By interacting with specific microbial fragments, the structural cells of the lungs: the fibroblasts: appear to develop a form of memory that can help them resist allergic inflammation.
For those of us working within Life Sciences & Innovation and NHS Strategy & Leadership, this discovery opens a significant conversation about pathway innovation and how we might approach long-term respiratory health.
Disclaimer: The information provided in this article is for informational purposes only and does not constitute medical advice. The Respiratory Network does not provide medical diagnoses or treatment recommendations. Always seek the advice of a qualified healthcare professional regarding any medical condition.
Moving Beyond the Immune System: The Role of Fibroblasts
Traditionally, the lung was viewed as a passive stage where the immune system performed its duties. We focused on T-cells, B-cells, and eosinophils. But the lungs are composed of structural cells, including epithelial cells and fibroblasts, which provide the organ's framework.
The study from the Pasteur Institute has highlighted that these fibroblasts are far from passive. They are active participants in the respiratory environment. Researchers found that when these cells are exposed to specific microbe fragments, they undergo a process of "epigenetic remodeling." Essentially, the "switches" in their DNA are adjusted, allowing the cells to remember the microbial encounter.
This "immune memory" in non-immune cells means that the lung structure itself can become "trained" to be less reactive to allergens. In practice, this suggests that the lung's physical environment plays a much larger role in determining whether a person develops chronic respiratory issues than previously thought.
The Gut-Lung Axis: A Systemic Connection
To understand how these microbes "teach" the lungs, we have to look beyond the chest cavity. The "gut-lung axis" is a critical pathway in respiratory health UK. The microbiota in our digestive system produce metabolites, specifically short-chain fatty acids (SCFAs) like butyrate and propionate.
These SCFAs act as messengers. They enter the bloodstream and travel to the lungs, where they have been observed to:
- Strengthen the epithelial barrier: Making it harder for allergens to penetrate the lung tissue.
- Modify fibroblast behavior: Reducing the synthesis of collagen that leads to airway remodeling and thickening.
- Dampen inflammation: Signalling to the local immune environment to remain in a "homeostatic" or balanced state rather than an over-reactive one.
What this looks like on the ground is a move toward a more holistic view of respiratory care. We are beginning to see that the diversity of a person's microbiome: shaped by diet, environment, and early-life exposure: is intrinsically linked to their lung's ability to resist the triggers that lead to asthma or severe hay fever.
The Critical Window of Opportunity
One of the most profound insights from this microbial research is the importance of timing. There appears to be a "critical window" in early childhood where this microbial training is most effective.
Data suggests that children raised in environments with high microbial diversity: such as farms or households with pets: often have a lower incidence of respiratory allergies. This is often referred to as the "hygiene hypothesis," but the new research provides a molecular explanation: their lungs have been effectively "trained" by early exposure to microbial fragments.
Conversely, factors that disrupt this early training: such as the over-prescription of antibiotics or limited exposure to diverse environments: can leave the lung fibroblasts "uneducated." Without this training, the structural cells are more likely to signal a high-alert inflammatory response when they eventually encounter pollen, dust mites, or animal dander.

Implications for NHS Strategy and Pathway Innovation
For NHS clinical leads and Life Sciences directors, these findings are more than just biological curiosities. they represent a potential shift in NHS Strategy. If we can understand the mechanisms of "lung training," we can begin to look at preventative pathway innovation.
1. Re-evaluating Prevention
Currently, much of our respiratory strategy is reactive, focusing on managing symptoms once a patient has already developed a condition. Insight into microbial training suggests a future where we might focus on supporting a healthy microbiome in early life to prevent the onset of allergic airway disease.
2. Diagnostics and Data
If the "memory" of these cells is held in their epigenetic state, there is a future where diagnostics could potentially identify which patients are at the highest risk of developing severe allergies based on their lung’s "training" history or their gut microbiome composition.
3. Integrated Care
This research reinforces the need for Integrated Care Systems (ICS) to work across disciplines. Respiratory health is not just the remit of the chest clinic; it involves nutrition, environmental policy, and primary care's approach to early childhood health.

What Patients and Clinicians Often Describe
When we speak to those with lived experience of asthma and severe allergies, they often describe a sense of their body "overreacting" to the smallest environmental changes. This new research validates that feeling. It isn't just an "overactive immune system"; it is a structural environment that has not been conditioned to tolerate common antigens.
Clinicians working under pressure in NHS Respiratory Services see the results of this daily: the seasonal spikes in admissions during "pollen bombs" or the high rates of asthma in urban areas with low biodiversity. Understanding the "lung training" mechanism provides a scientific framework for why some patients are so much more vulnerable than others, even when their clinical presentations appear similar.
Moving Forward: A Collaborative Effort
The concept of microbial training is still largely in the realm of advanced research, but its trajectory is clear. We are moving toward a more nuanced, personalized, and preventative model of respiratory care.
In the UK, the challenge is to bridge the gap between this high-level science and the practical reality of the NHS. This requires a strong partnership between Life Sciences, which develops the insights and potential interventions, and the NHS, which must integrate these findings into stressed clinical pathways.
At The Respiratory Network, we believe these conversations are essential. Whether you are a patient advocate concerned about the rising tide of allergies, a clinician looking for better ways to support your patients, or a Life Sciences leader driving the next wave of innovation, we all have a stake in how this science is applied.
Join the Conversation
The future of respiratory health depends on our ability to share these insights and turn them into actionable strategy. We invite you to be part of this mission.
- Become a Member: Join our growing community of professionals and patient advocates to stay updated on the latest clinical and strategic developments. Join here.
- Follow Us: Stay connected with us on social media for daily updates and insights into the UK respiratory landscape.
- Attend Our Next Event: We regularly host round tables and forums to discuss the intersection of science and strategy. Check our events page for upcoming dates.
By working together, we can ensure that "lung training" and other biological breakthroughs don't just stay in the lab, but lead to real-world improvements for everyone breathing in the UK.
Categories: Life Sciences & Innovation; Clinical Updates
Tags: Respiratory Health UK; Pathway Innovation; NHS Leadership; Life Sciences Engagement UK; Asthma; Diagnostics; NHS Strategy; Integrated Care Systems (ICS).







Responses